Process for Listing of Validated Blood Pressure Monitors
The BIHS Blood Pressure Measurement Working Party is responsible for maintaining an impartial list of validated blood pressure monitors on its website. The list is updated regularly with changes to the existing information and new devices.
The BIHS Validation Service for manufacturers of blood pressure monitors is suspended until further notice due the COVID-19 pandemic. This will be reviewed in due course.
For successful validation studies performed on devices by other agencies, the procedure for inclusion in the BIHS list of validated blood pressure monitors, is as follows:
An independent validation should be undertaken and passed using at least one of the following testing standards:
2 ESH International Protocol 2002 (IP1)
3 EHS International Protocol 2010 (IP2)
4 Universal Standard for the validation of blood
pressure measuring (AAMI/ESH/ISO) 2019
The full report of the validation study, describing the process and results should be published in a peer-reviewed journal. The Working Party is not obliged to suggest journals in which the validation paper should be published nor by whom the validation should be undertaken but this should be independent of the manufacturer.
The manufacturer may submit an electronic copy of the full published paper (abstracts will not be accepted) to bihs@in-conference.org.uk for review by the Working Party prior to any decision on listing being made. There is no charge for this service and members of the Working Party provide their services voluntarily. Therefore, a time-schedule for a decision cannot be given.
Validated devices will be added to the BIHS website list under the most appropriate category heading. Where monitors have been only tested in a specific area, such as pregnancy, this will be clearly stated on the website.
The BIHS logo cannot be used on devices tested by independent agencies.
BIHS statement on Derivative Devices 2023
Devices that are listed as being derivative of other models have been approved for addition to these lists on the basis of information supplied to the BIHS by the manufacturer. This comprises a checklist of the key components of each monitor (including algorithm, pressure sensors, cuff size and construction, inflation/deflation processes) which the manufacturer attests have not been materially changed from the originally validated device. This information has been carefully reviewed, with manufacturers’ attestations accepted in good faith. Derivative devices are indicated on the list and the original model name is given in brackets.
From 1st April 2023, the BIHS will only accept new derivative device applications where the original device validation was carried out under the European Society of Hypertension International Protocol revision 2010[1] or AAMI 2013 onwards or the Universal Standard (AAMI/ESH/ISO) validation protocol 2018[2,3,4]. This is because the 2002 ESH International Protocol and earlier protocols (including BIHS 1993) will be considered obsolete from then onwards.
From 1st April 2025, the BIHS will only accept new derivative device applications where the original device validation was carried out under the 2018 Universal Standard (AAMI/ESH/ISO) protocol or a subsequent modification of that protocol.
Validations carried out with other protocols subsequent to 2018 (including but not limited to subsequent AAMI protocols) may be accepted at the discretion of the BIHS but manufacturers should check in advance of any submission.
References:
[1] Blood Pressure Monitoring 2010, 15:23–38
[2] Hypertension 2018; 71:368–374
[3] Journal of Hypertension 2019, 37:459–466
[4] https://www.aami.org/store/aami-products/1
Application for Listing a Derivative of a Validated BP Monitor
In order to cover administrative costs, the BIHS will henceforth levy a charge for all Derivative Device applications. The fee (£600 + VAT) is non-refundable should the application be rejected. The Blood Pressure Measurement Working Party will make every effort to process applications within 4 weeks of receipt. For further details, email bihs@in-conference.org.uk
To download the application form click here
What determines the accuracy of the blood pressure measurement device?
Implications for device equivalence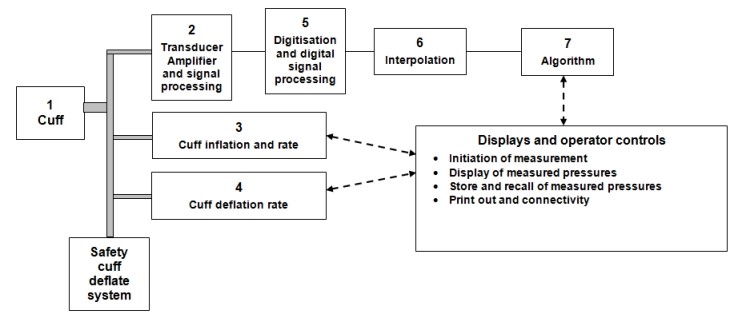
Figure: Simplified block diagram of an Automated non-invasive blood pressure measuring device
The accuracy of the device depends on the cuff; the transducer that records the cuff pressure and the amplifier and signal processing (e.g. some form of filter) that records the cuff pressure; the digitisation and subsequent digital signal processing that extract the oscillometric pulses; interpolation between sampled pulses and the algorithm used to analyse the oscillometric pulses and their variation with cuff pressure. The rate of change of cuff pressure during the measurement phase will affect measurement accuracy (traditionally during linear cuff deflation, but step deflation and measurement during inflation are also used). The inflation of the cuff (assuming measurement during cuff deflation) can also affect accuracy, for example dependent on the difference between the pressure that the cuff is inflated to and the systolic pressure.
Thus in declaring equivalence, manufacturers should state, with reference to the block diagram, if there are any changes in any of the numbered functional blocks:
1. Cuff characteristics
2. Transducer, amplifier and any signal processing carried out prior to digitisation
3. Cuff inflation.
4. Cuff deflation.
5. Digitisation (sampling frequency and number of bits), and digital signal processing
6. Interpolation. The oscillometric pulses occur only every heart beat and it is not uncommon for designers to interpolate between pulses to increase the accuracy and reduce the measurement variability whilst increasing the cuff deflation rate (or inflation rate for those devices that measure during cuff inflation) to reduce the measurement time.
7. Algorithm